-
About
- Leadership & Faculty
- News & Events
-
Academics
- Graduate
- Advanced Clinical Training
- Continuing Education
-
Student Life
- Graduate Programs
-
Research
-
Hospitals & Clinics
- Emergency Care
-
Community Outreach
- Volunteer
Collaboratively Cured
Internal medicine and dermatology teams work together to help Palomino with pemphigus foliaceus
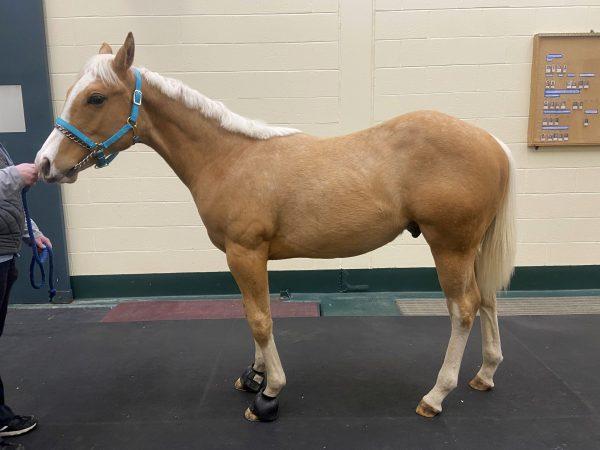
When Bonnie Lowell picked up Maxx, a six-month-old Palomino colt, from a breeder in Georgia in early December, he was suffering from suspected rain rot (a bacterial skin infection), with swollen legs and scabs that covered his entire body. After returning home, Bonnie immediately called the veterinarian. Bloodwork suggested a bacterial infection. Maxx started on a course of antibiotics, but his symptoms did not abate over the next several days.
“Maxx never wanted to trot, never offered to do any of the typical baby antics like running, bucking, rearing,” Lowell laments.
Lowell has chickens, goats, oxen, cats, Labradors, and horses on her small farm in Southbridge and Dudley, Massachusetts, and had previously taken her other horses to the Hospital for Large Animals (HLA) at Cummings School of Veterinary Medicine at Tufts University. After Maxx spiked fevers over the following week, Bonnie brought him to HLA.
Lauren Holley, a resident in large animal internal medicine, Daniela Bedenice, associate professor and a specialist in internal medicine and critical care of large animals, and Ekaterina Mendoza-Kuznetsova, dermatology specialist and clinical assistant professor, led the teams treating Maxx.
“The most striking findings were the patchy skin lesions all over his body. Also, for a foal his age, he didn’t have normal muscle mass and his appearance was more scruffy-looking,” admits Holley. “His legs had lost all their contour and they were so swollen due to inflammation.”
Maxx was taken to the HLA quarantine facility due to the undetermined nature of his fever. Based on the colt’s recent history, lack of response to appropriate prior treatment, and his overall clinical presentation, an immune-mediated condition was suspected, which can have a variety of infectious or noninfectious causes.
A full physical exam, including bloodwork, radiographs of his lungs, ultrasound of his chest and abdomen, and endoscopy of his upper airways and guttural pouches, were performed to identify any underlying source of infection that could have triggered an immune-mediated disease. The doctors found worms in his gut and high inflammatory markers, but no signs of other infections.
The dermatology team took skin cytology samples and skin biopsies that confirmed the diagnosis of pemphigus foliaceus (PF), an autoimmune disorder that causes horses to develop antibodies against specific layers of their own skin, leading to sores, scaling, and crusting. Although PF is usually not painful, the associated sores and inflammation can cause discomfort and itching.
“Pemphigus can be a severe disease and it is not uncommon that horses have to be humanely euthanized, either due to the disease itself or medical complications that develop following treatment,” Bedenice explains, adding that younger horses may respond better than older horses with PF and can stay in remission after treatment is withdrawn.
PF is the most common autoimmune skin disease in horses, but it is still fairly rare. PF’s causes are not entirely known and may be different for each patient. Holley explained that typically a trigger, such as an insect bite, infection, a certain drug or vaccine, for example, sets off the immune system inappropriately. Genetic factors and stress (such as weaning a foal) may also contribute to the development of PF.
A joint effort between the internal medicine and dermatology teams at the Hospital for Large Animals put Maxx on the road to recovery.
“The specialties work together often—and it shows excellent teamwork,” says Holley. “The dermatology, neurology, ophthalmology, and cardiology teams can be consulted for medical patients and bring very specific expertise to treat the whole animal.”
The doctors started a tapering course of immunosuppressant steroids to treat Maxx’s autoimmune condition. He also began a slow-kill deworming protocol, shampoos for his coat to stop the itchiness, and controlled exercise to address the swelling in his legs.
“Steroids in themselves represent a difficult challenge in horses because they can have serious complications that you don’t see in smaller species,” Holley shares. Under certain circumstances, steroids may cause inflammation of the feet or ‘founder.’
“Horses essentially live and die on their feet, so we have to be careful how we use steroids. We start with the lowest dose that is effective and gradually taper patients off medication, if possible.”
Maxx returned home after spending two days at HLA. Within two weeks, the swelling in his legs and the smaller scabs disappeared. Lowell sends Holley weekly updates and images of Maxx’s progress.
“The doctors’ communication with me has been incredible,” Bonnie says. “They make me feel like we’re going to get through this with Maxx, and hopefully we’ll have a normal horse after this. They give us as much information as they can for this rare disease and give me hope for his future.”
The goal of treatment is to put the disease into remission and reach a point where Maxx does not need steroids and does not relapse.
“The change from the beginning is drastic,” Holley explains. “The leg swelling is gone, he’s growing muscle, and looking much more like a foal his age.”
When Maxx returned to HLA at the end of April for a check-up, Mendoza-Kuznetsova reported, “Maxx is doing great. He has been off his medications for three weeks and does not have any relapse. We hope his condition is cured.”
“It is very helpful having the support of every department at Tufts,” Bonnie contends. “It’s one stop. Everybody you might need to see is there. Internal medicine, dermatology—they have the resources to weigh in and work with us. Tufts is fabulous.”
Department:
Foster Hospital for Small Animals